Center of Excellence Advances Precision Lung Surgery via Mobile CT
During lung tumor or nodule surgery, patients are often required to travel from their hospital wards to the Radiology Department’s CT suite on the day of the operation. A localization needle is inserted through the skin. Although the procedure is performed under local anesthesia, patients remain awake and frequently experience anxiety and physical discomfort. In addition, the wait time between localization and surgery can be long. During this process, some patients develop pneumothorax or hemothorax, leading to shortness of breath or chest pain. In severe cases, an emergency drainage tube must be inserted.
Taipei Veterans General Hospital (TVGH) thoracic surgery team has redesigned the workflow to improve this situation. Aside from the traditional CT-guided localization, the team utilizes an electromagnetic navigation system, mobile CT, and hybrid operating rooms (hybrid OR). The combined electromagnetic navigation with mobile CT in the hybrid OR allows localization and surgery to be completed one-stop by the thoracic surgeon in the operating room, reducing patient discomfort and risks associated with transport and waiting.

Reducing Patient Radiation Exposure with Electromagnetic Navigation
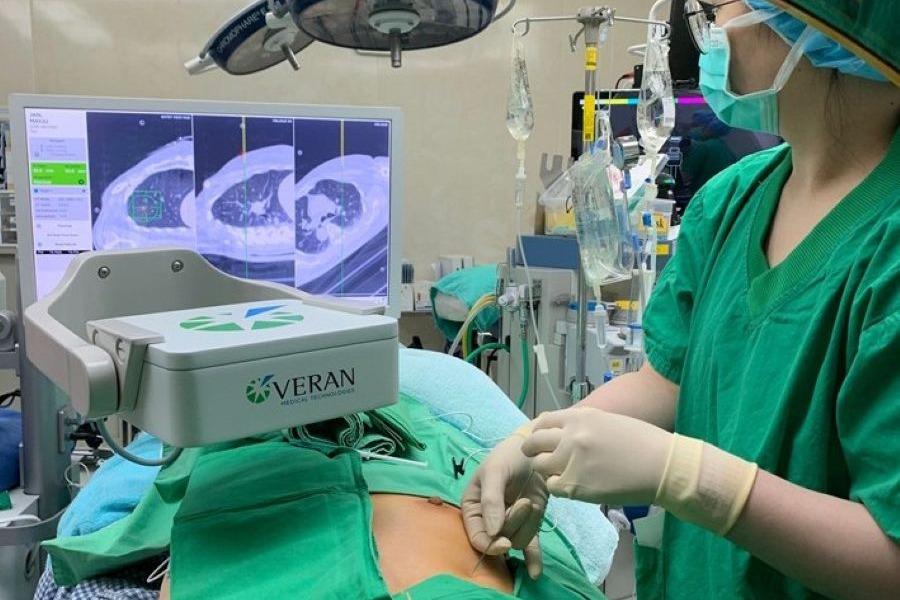
Yi-Ying Lee, an attending physician at TVGH Thoracic Surgery, explains that when using the Electromagnetic Navigation system, doctors perform preoperative planning, similar to mapping out a route before driving. On the day of the surgery, a CT scan is performed (for imaging only, no needles are inserted), and sensing patches are applied to the patient's chest. These images serve as the "map" for the surgery.
Once the patient is anesthetized in the OR, the doctor follows this map. During the procedure, an electromagnetic generator creates a magnetic field that detects the patches on the patient and the sensor in the doctor’s localization needle.
This allows the surgeon to track the patient's breathing and lesion movement in real-time. Another advantage of ENS is that patients are not exposed to radiation during the localization process, and it can be paired with non-intubated anesthesia for specific cases.
Po-Kuei Hsu notes that TVGH was the first in Taiwan to introduce ENS in 2018. In 2020, the hospital was certified as the first Electromagnetic Navigation Center of Excellence in Asia, placing its technology at the forefront of the region.
Mobile CT Reduces Patient Transport Risks
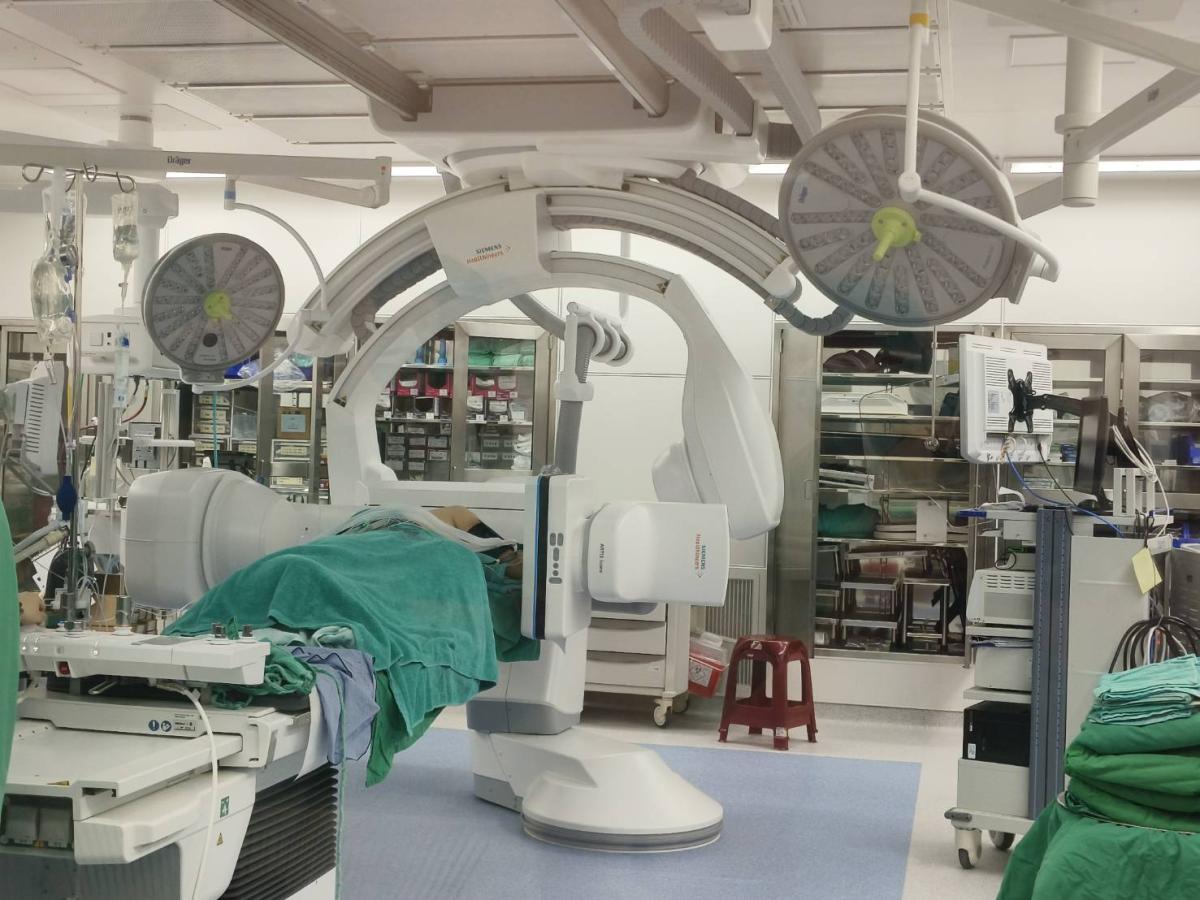
In addition to electromagnetic navigation system (ENS), TVGH introduced the only Mobile CT currently available in Taiwan. Han-Shui Hsu, Director of Thoracic Surgery, states that TVGH is one of the few hospitals globally and the first in Taiwan to use Mobile CT for lung lesion localization. This mobile unit provides high-quality real-time imaging and can be moved between operating rooms for use in orthopedics or neurosurgery as well.
Yi-Ying Lee adds that while the technology is similar to traditional CT, the clinical benefit is significant. By moving the localization process from the Radiology Department to the OR, thoracic surgeons can perform the localization themselves. This eliminates the risk and stress of transporting the patient between different departments while a needle is lodged in their chest.
Improved Accuracy with Electromagnetic Navigation and Mobile CT-Guided Localization
With the help of Mobile CT, the TVGH team can now perform "dual confirmation" when using ENS. Lee explains that because the lungs shift during inhalation and exhalation, they use the Mobile CT to perform a localized scan after the ENS localization. This confirms the exact relative position of the needle tip and the lesion, minimizing errors caused by respiratory movement.
TVGH now has a state-of-the-art Hybrid OR equipped with an integrated CT scanner. "We have virtually every localization method currently available to physicians in Taiwan," says Dr. Han-Shui Hsu. He notes that in the past, patients had to remain awake during localization in the radiology CT room, which caused pain and distress.
“Our goal is for patients to be under general anesthesia and have the localization performed directly in the operating room to minimize discomfort.”
The TVGH thoracic surgery team is a strong advocate for precision localization. "Our objective is to have the same patient, in the same location (the OR), treated by the same medical team for both localization and surgery, as we are the ones who understand that patient best," says Po-Kuei Hsu.
Yi-Ying Lee adds that this one-stop technique allows patients to go directly from the ward to the operating room, undergo both localization and surgery, and then return straight to the ward. The entire process from localization to the completion of surgery takes only about 30 minutes, significantly reducing the time spent on bed transfers and waiting.
"The goal is to have the same patient, in the same place (the OR), treated by the same medical team for both localization and surgery, because we understand that patient best," says Po-Kuei Hsu. This one-stop approach allows a patient to go from the ward to the OR and back to the ward in a significantly shorter timeframe, with the actual procedure taking about 30 minutes from localization to completion.
Non-Intubated Anesthesia Minimizes Complications
The team has also innovated in surgical techniques, aiming for smaller incisions and "tubeless" procedures. Traditional thoracoscopic surgery requires general anesthesia with a thick double-lumen endotracheal tube to collapse one lung. Now, the Anesthesiology Department can perform non-intubated thoracoscopic anesthesia. This avoids potential damage to the vocal cords and reduces complications like hoarseness.
Hsu describes the sensation as similar to undergoing a painless gastroscopy—the patient sleeps and breathes naturally while the surgeon operates. This requires anesthesiologists to exert more effort in monitoring and fine-tuning the patient’s respiratory rate. Overall, patients require less medication and recover faster.
Surgical Intervention Across All Lung Cancer Stages
With continuous breakthroughs in medical technology, thoracic surgeons now play a vital role across all stages of lung cancer. For patients in Stages I and II, surgery remains the core curative treatment, though recent trials suggest that combining chemotherapy and immunotherapy before surgery for Stage II patients can help break through previous treatment bottlenecks.
In cases of early-stage III lung cancer, surgery is typically the first choice; however, if the tumor size or the patient’s lung function makes immediate surgery risky, systemic treatments, such as chemotherapy, radiation, targeted therapy, or immunotherapy, are utilized first. Surgery is then re-evaluated once the lesion has shrunk and the patient's condition has stabilized.
For patients with late-stage or advanced lung cancer, the medical consensus is shifting toward using systemic therapies as "induction" to shrink tumors before proceeding with surgical resection. This integrated approach often yields better clinical results than relying solely on long-term medication, offering new hope and improved survival outcomes for advanced-stage patients.
Consequently, the role of the thoracic surgeon is no longer limited to early-stage intervention but has become an essential part of a multidisciplinary strategy to create more opportunities for recovery at every stage of the disease.
Editor's note: This article features the Bronze Award recipient of the 25th National Biotechnology and Medical Quality Award (2023), Healthcare Institution Category – Featured Medical Services. All titles and positions mentioned reflect the interviewees’ roles at the time of the interviews.






